https://doi.org/10.55788/1546ab9d
Although in the past years there has been an increase in available anti-seizure medications, drug-resistance in epilepsy patients has not decreased. An Italian study, presented by Dr Giovanni Falcicchio (University Hospital of Bari "A. Moro", Italy), investigated cenobamate as adjunctive treatment for patients with uncontrolled FOS [1]. Included were 20 adult patients who were enrolled in an Italian Expanded Access Program (EAP) with uncontrolled FOS and no treatment alternatives. Collected were efficacy and safety data 3, 6, and 12 months after administration of cenobamate, along with plasma concentrations of concomitant anti-seizure medication. Primary efficacy outcomes were median percentage change in monthly seizure frequency and responder rate (≥50% monthly seizure frequency reduction).
After 3 months, participants taking cenobamate reported a significant reduction (mean 63%) in seizure frequency compared with baseline, with a responder rate of 11/20 (58%). At month 6 and 12, decrease in seizure frequency was sustained. Adverse events were reported in 16 patients (80%), mainly mild and transient, and generally disappeared after reducing the posology of other anti-seizure medication the patient was taking.
Safety and efficacy of cenobamate as adjunctive therapy in an early-access programme was also assessed in a Spanish case series [2]. This prospective, longitudinal, multicentre study, presented by Dr Ariadna Gifreu (Bellvitge University Hospital, Spain), included 58 adult patients with drug-resistant epilepsy (mean age 40 [range 19–70]; 31 women). Median number of previous and concomitant anti-seizure medications were 9 and 3, respectively. Median monthly seizure frequency at baseline was 8.5 (range 5–30). Responder rates (≥50% monthly seizure frequency reduction), seizure free rates, and retention rates were measured at 6 months; adverse events (AE) at 3 and 6 months.
Median dose at 6 months was 200 mg/day (range 75–400 mg/day). At 6 months, median seizure frequency per month decreased significantly from 8.5 to 4 (P<0.001). Of 44 participants, 26 (59%) were responders (see Figure for all responder rates). Retention rate was 41 out of 47 participants (87%). Of 58 patients, 36 (62%) experienced AEs during the titration period and 25 out of 44 (57%) after 6 months.
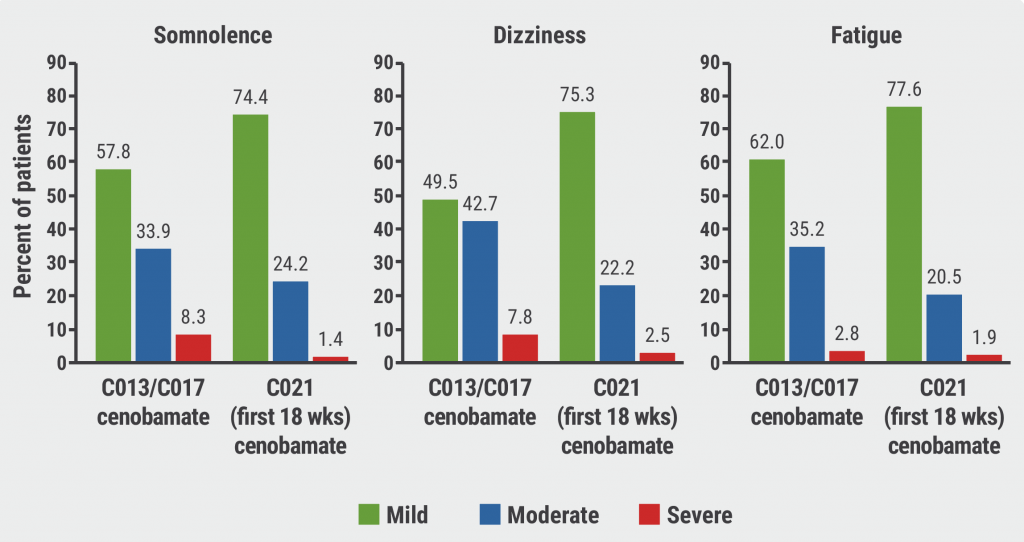
The most common AEs were somnolence, unsteadiness, and dizziness. There were no serious AEs.
Figure: Responder rates at 6 months for seizure frequency reduction >50%, >90%, and seizure-free [2]

- Falcicchio G, et al. Cenobamate: preliminary results of efficacy and safety in a real-life setting. OPR-077, EAN 2022, 25–28 April, Vienna, Austria.
- Gifreu A, et al. Short term efficacy and safety of adjunctive cenobamate in patients with super-refractory focal epilepsy. OPR-082, EAN 2022, 25–28 April, Vienna, Austria.
Copyright ©2022 Medicom Medical Publishers
Posted on
Previous Article
« Possible new biomarker for early neuronal death in mesial temporal lobe epilepsy Next Article
Seizure forecasting with non- and minimally-invasive devices »
« Possible new biomarker for early neuronal death in mesial temporal lobe epilepsy Next Article
Seizure forecasting with non- and minimally-invasive devices »
Table of Contents: EAN 2022
Featured articles
Letter from the Editor
Overarching Theme
Migraine
Targeting cortical activation by transcranial magnetic stimulation
Erenumab more than doubles plasma CGRP levels
Over a third of patients responds late to CGRP antibodies
Multiple Sclerosis
When to start, switch, and stop MS therapy: Real-world evidence counts
Updated EAN-ECTRIMS guideline on pharmacological MS treatment
Gut microbiota composition associated with disability worsening
Teriflunomide in children with MS: final results of TERIKIDS
Estimating brain age in MS: machine learning versus deep learning
Ofatumumab improves cognitive processing speed
Parkinson’s Disease
Intestinal alterations in patients with Parkinson’s disease
Gene variants impact survival in monogenic Parkinson’s disease
Cerebrovascular Disease and Stroke
Most acute stroke patients have undiagnosed risk factors
Absence of Susceptibility Vessel Sign points to malignancy in stroke patients
Acute stroke management: from time window to tissue window?
Epilepsy
Seizure forecasting with non- and minimally-invasive devices
Real-world efficacy of cenobamate in focal-onset seizures
Possible new biomarker for early neuronal death in mesial temporal lobe epilepsy
COVID-19
COVID-19 elevates risk of neurodegenerative disorders
More headaches in adolescents during COVID-19 pandemic
AstraZeneca vaccination and risk of cerebral venous sinus thrombosis
Large impact of COVID-19 on dementia diagnosis and care
Miscellaneous
Tau autoimmunity associated with systemic disease
Long-term effects of avalglucosidase alfa in late-onset Pompe disease
European survey of patient satisfaction in the treatment of cancer-related neuropathic pain
Related Articles
August 18, 2021
Good safety and efficacy of cenobamate for focal seizures
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy
HEAD OFFICE
Laarderhoogtweg 25
1101 EB Amsterdam
The Netherlands
T: +31 85 4012 560
E: publishers@medicom-publishers.com

