Primary outcomes were successful recanalisation, defined as modified thrombolysis in cerebral infarction (mTICI 2b-3), good outcome at 3 months according to modified Rankin scale (mRS; 0-2 or back to baseline), and rates of intracranial haemorrhage (ICH) until hospital discharge.
The analysis included 2,521 stroke patients, of whom 442 (17.6%) were treated with OACs, 201 (8.0%) with vitamin-K antagonists (VKA), and 241 (9.6%) with non-vitamin-K antagonist oral anticoagulants (NOACs). OAC users were older, had more often a history of atrial fibrillation, and had a higher rate of arterial hypertension (see Table).
The rate of mTICI 2b-3 was similar among all 3 groups (82.7%, 85.5%, and 82.7%; P=1.00 and P=0.57). The other main results after 90 days:
- A favourable outcome was less frequent in OAC patients (28.4%, 31.1%, and 40.9%; P<0.005 and P<0.05);
- ICH rates were similar among the 3 groups (12.1%, 12.4%, and 10.4%; P=1.00 and P=0.86);
- OAC status had no influence on good outcome (OR 1.03; 95% CI 0.99-1.08);
- OAC status did not affect ICH risk (OR 1.03; 95% CI 0.94-1.05).
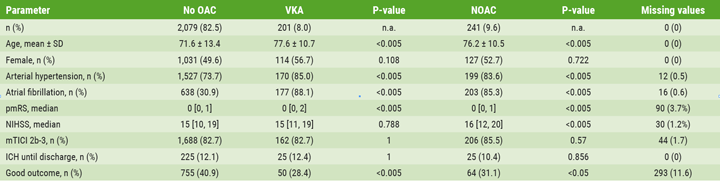
OAC, oral anticoagulation; VKA, vitamin-K antagonist; NOAC, non-vitamin-K oral anticoagulant; pmRS, premorbid modified Rankin Scale; NIHSS, National Institute of Health Stroke Scale; mTICI, modified thrombolysis in cerebral infarction; ICH, intracranial haemorrhage
- Küpper C, et al. Abstract EPR2022, EAN 2020.
Posted on
Previous Article
« Early edoxaban may be safe after cardioembolic stroke Next Article
Thrombus location and length predictors of early neurological deterioration »
« Early edoxaban may be safe after cardioembolic stroke Next Article
Thrombus location and length predictors of early neurological deterioration »
Table of Contents: EAN 2020
Featured articles
Alzheimer's Disease and Other Dementias
Non-Alzheimer’s disease pathophysiology in the elderly
Novel genetic association with resistance to ERC tau deposition
Diastolic dysfunction novel risk factor for cognitive impairment
Epilepsy
Avoidable epilepsy-related mortality remains high
How genetic testing can contribute to epilepsy management
Cenobamate effective in focal epilepsy
Sustained seizure reductions with cannabidiol for Lennox-Gastaut syndrome
Prevalence of autoantibodies in epilepsy almost 10%
Parkinson's Disease
White matter matters in Parkinson’s disease
Sleep disorders mark PD progression
Directional DBS superior to omnidirectional DBS
Stroke
Benefits of statins to prevent stroke outweigh risks
Extubation after thrombectomy: the sooner, the better
Thrombus location and length predictors of early neurological deterioration
Endovascular treatment in large vessel occlusion stroke patients treated with OAC
Early edoxaban may be safe after cardioembolic stroke
Headache and Pain
Small fibre pathology as biomarker for fibromyalgia
Migraine as a cyclical functional disorder
Reassuring real-world safety profile of 3 CGRP inhibitors
Long-term cardiovascular safety of erenumab
Real-world data for erenumab in Germany
Eptinezumab in chronic migraine and medication-overuse headache
Fremanezumab tolerability in cardiovascular patients with migraine
Effects of galcanezumab on health-related quality of life
Multiple Sclerosis
Imaging to evaluate remyelination and neuroprotection
Serum NfL predicts long-term clinical outcomes in MS
Epstein-Barr virus-targeted T-cell immunotherapy for progressive MS
High NEDA rates after 2 years of ocrelizumab
Switching from natalizumab to moderate- versus high-efficacy DMT
Results of compounds in late stages of development
Alemtuzumab efficacy and safety data of over 9 years
Fampridine treatment results in routine clinical practice
Air pollution is a possible risk factor for MS
Neuromyelitis Optica Spectrum Disorder
Genetic association studies in NMOSD needed
Eculizumab in NMOSD: the PREVENT study
Long-term safety of satralizumab consistent with double-blind periods
Neuromuscular Disorders
Biomarkers predicting motor function in SMA
Sustained benefits of avalglucosidase alfa in late-onset Pompe disease
Efficacy and safety of rituximab in refractory MG corroborated
Related Articles
September 9, 2020
Real-world data for erenumab in Germany
September 10, 2020
High NEDA rates after 2 years of ocrelizumab

September 10, 2020
Imaging to evaluate remyelination and neuroprotection
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy

