https://doi.org/10.55788/36e81ef6
Adding an EGFR inhibitor or VEGF inhibitor to chemotherapy improves the overall survival (OS) of patients with mCRC significantly [1]. In patients with RAS wildtype, left-sided, colorectal tumours, the benefit of an EGFR inhibitor may be enriched, based on retrospective analysis [2]. The phase 3 PARADIGM trial assessed this matter by randomising 823 patients with RAS wildtype mCRC 1:1 to mFOLFOX6 plus the EGFR inhibitor panitumumab or to mFOLFOX6 plus the VEGF inhibitor bevacizumab [3]. In total, 604 patients had left-sided tumours. The primary endpoints of this trial were OS in the left-sided population and OS in the overall population. Dr Takayuki Yoshino (National Cancer Center Hospital East, Japan) presented the results.
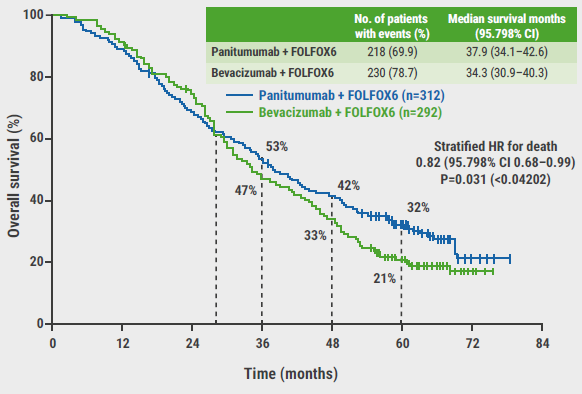
After 5 years of follow-up, panitumumab performed better than bevacizumab in terms of median OS in both the left-sided population (37.9 vs 34.3 months; HR 0.82; P=0.031; see Figure) and the overall population (36.2 vs 31.3 months; HR 0.84; P=0.030). The OS curves of the 2 treatment regimens separated after 28 months. In contrast, the median progression-free survival did not differ between treatment regimens: left-sided population (13.7 vs 13.2 months; HR 0.98); overall population (12.9 vs 12.0 months; HR 1.01). According to Dr Yoshino, the research group expected this result. Other efficacy outcomes favoured the panitumumab arm, especially in the left-sided sub-population, in whom response rates were 80.2% versus 68.6%. Interestingly, an exploratory analysis of OS in the right-sided population did not display a benefit of panitumumab over bevacizumab (20.2 vs 23.2 months; HR 1.09).
Figure: Overall survival of panitumumab versus bevacizumab in left-sided population [3]
No new safety issues were observed for the treatment regimens. In the panitumumab arm, 71.8% of the patients experienced grade ≥3 adverse events compared with 64.9% of the patients in the bevacizumab arm. The treatment discontinuation rates due to adverse events were 23.8% and 18.4% in the panitumumab arm and bevacizumab arm, respectively. Acne-like dermatitis, paronychia, dry skin, and hypomagnesaemia were more often observed in patients on panitumumab.
“These results support panitumumab plus mFOLFOX6 as first-line therapy for patients with RAS wildtype and left-sided mCRC,” concluded Dr Yoshino. “A large-scale biomarker analysis is currently ongoing (NCT02394834) to gain in-depth understanding of these results.”
- Venook AP, et al. JAMA. 2017;317(23):2392‒2401.
- Arnold D, et al. Ann Oncol. 2017; 28(8):1713‒1729.
- Yoshino T, et al. Panitumumab (PAN) plus mFOLFOX6 versus bevacizumab (BEV) plus mFOLFOX6 as first-line treatment in patients with RAS wild-type (WT) metastatic colorectal cancer (mCRC): Results from the phase 3 PARADIGM trial. LBA1, ASCO 2022 Annual Meeting, 3–7 June, Chicago, IL, USA.
Copyright ©2022 Medicom Medical Publishers
Posted on
Previous Article
« Spectacular results for dostarlimab in mismatch repair deficient rectal cancer Next Article
Encouraging results of relacorilant in ovarian cancer »
« Spectacular results for dostarlimab in mismatch repair deficient rectal cancer Next Article
Encouraging results of relacorilant in ovarian cancer »
Table of Contents: ASCO 2022
Featured articles
Breast Cancer
Sacituzumab govitecan meets primary endpoint
Shaky OS results of palbociclib in ER-positive/HER2-negative breast cancer
Practice-changing results of T-DXd in HER2-low breast cancer
SET2,3 to inform on chemotherapy decisions in ER-positive breast cancer
Metastasis-directed therapy fails in oligometastatic breast cancer
Analysis by residual cancer burden further clarifies effect of pembrolizumab
Contribution of metastatic therapies on mortality reduction in breast cancer
Radiotherapy may be omitted in breast cancer patients
Promising data for ribociclib after progression on ET plus CDK4/6 inhibitors in HR-positive/HER2-negative metastatic breast cancer
7-gene biosignature: Benefits of endocrine therapy and radiotherapy in breast cancer risk groups
Lung Cancer
Additional tiragolumab does not help patients with untreated small cell lung cancer
Success for serplulimab plus chemotherapy in small cell lung cancer
Adagrasib safe and clinically active in non-small cell lung cancer
Long-term benefits of combined immunotherapy over chemotherapy in non-small cell lung cancer
Effect of KRAS mutations and PD-L1 expression on therapy response in non-small cell lung cancer
Melanoma
First results on distant metastasis-free survival in stage II melanoma
Higher response rates for concurrent triple therapy versus sequential therapy in melanoma
Genitourinary Cancers
Exploratory treatment options fail in ccRCC
Adjuvant everolimus did not benefit high-risk renal cell carcinoma
Cabozantinib fails as first-line maintenance therapy in urothelial cancer
177Lu-PSMA-617 is a valid treatment option for PSMA-positive mCRPC
Enzalutamide performs well in metastatic hormone-sensitive prostate cancer
Haematologic Malignancies
Autologous stem cell transplantation plus RVd improves PFS in multiple myeloma
Novel first-line treatment option for mantle cell lymphoma
Promising results for novel CAR-T therapy in relapsed/refractory multiple myeloma
Gastrointestinal Cancers
Panitumumab beats bevacizumab in RAS wildtype left-sided metastatic colorectal cancer
Spectacular results for dostarlimab in mismatch repair deficient rectal cancer
Triplet chemotherapy beats doublet chemotherapy in colorectal cancer liver metastases
To resect or not to resect primary tumours in stage IV colon cancer?
Novel treatment option for KRAS wildtype pancreatic cancer
Gynaecological Cancers
Primary results of rucaparib in ovarian cancer
Trabectedin not superior to chemotherapy in recurrent epithelial ovarian cancer
Encouraging results of relacorilant in ovarian cancer
Miscellaneous Topics
Bacterial decolonisation effective against radiation dermatitis
New standard-of-care for cisplatin-ineligible locally advanced head and neck squamous cell carcinoma
Ifosfamide is likely to be the go-to therapy in recurrent Ewing sarcoma
Dabrafenib plus trametinib candidates for standard-of-care in BRAF V600-mutated paediatric low-grade glioma
Related Articles
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy

