Prof. Julio Nuñez Villota (University Clinical Hospital of Valencia, Spain) explained that within the multiple pathophysiological mechanisms that are implicated in the heterogeneous syndrome of HFpEF, chronotropic incompetence plays a crucial role in some patients [1]. “Despite the lack of robust evidence, most HFpEF patients are currently treated with renin-angiotensin-aldosterone system (RAAS) inhibitors or β-blockers,” he stated. In recent large HFpEF trials, 70–80% of patients received β-blocker medication [2]. With this in mind, the aim of the PRESERVE-HR trial (NCT03871803) was to assess whether β-blocker withdrawal would lead to a short-term improvement in functional capacity in patients with HFpEF [1].
The crossover, investigator-blinded, randomised PRESERVE-HR trial included 52 patients with a left ventricular ejection fraction (LVEF) ≥50% and an N-terminal pro B-type natriuretic peptide (NT-proBNP) of >125 pg/mL. Furthermore, all subjects had had a previous hospital admission for acute heart failure, were stable on β-blockers for ≥3 months, and had established chronotropic incompetence with an index of <0.62. Exclusion criteria included a resting heart rate of over 75 at screening. Baseline characteristics showed a mean age of 74.5 years, 59.6% women, 88.5% patients with hypertension, 34.6% in NYHA class III or IV, mean LVEF was 64.7%, and median NT-proBNP 400 pg/mL [1]. “Regarding the exercise test parameters, the mean peak VO2 was 12.5 mL/kg/min, percentage of predicted peak VO2 was approximately 72%, and the chronotropic index was 0.41, reflecting chronotropic incompetence. Importantly, there were no significant differences between both treatment arms,” commented Prof. Nuñez.
All participants underwent cardiopulmonary exercise testing (CPET) with cycle-ergometry at days 0, 15, and 30 of the trial. Study arm A started with β-blocker withdrawal and crossed over to a re-introduction of β-blocker therapy after 15 days, while arm B stayed on β-blockers for the first part of the study and withdrew β-blockers in the second part. The primary endpoint was defined as change from baseline peak VO2 and percentage of predicted peak VO2. Among the secondary endpoints were differences in biomarkers, health status assessment, cognitive function, and specific echocardiographic measures [1,3].
- Nuñez Villota J. Effect on Maximal Functional Capacity of Betablockers Withdrawal in Heart Failure with Preserved Ejection Fraction and Chronotropic Incompetence: PRESERVE-HR trial. LBT 3, Heart Failure and World Congress on Acute Heart Failure 2021, 29 June–1 July.
- Meyer M, et al. Circ Heart Fail. 2019;12(8):e006213.
- Palau P, et al. Clin Cardiol. 2020;43(5):423-429.
Copyright ©2021 Medicom Medical Publishers
Posted on
Previous Article
« Inconclusive results for dapagliflozin treatment in heart failure Next Article
Baroreflex activation: a novel option to improve heart failure symptoms »
« Inconclusive results for dapagliflozin treatment in heart failure Next Article
Baroreflex activation: a novel option to improve heart failure symptoms »
Table of Contents: HFA 2021
Featured articles
Inconclusive results for dapagliflozin treatment in heart failure
Late-Breaking Trials
Iron substitution improves LVEF in intensively treated CRT patients with iron deficiency
Novel mineralocorticoid receptor antagonist effective irrespective of HF history
Iron substitution in iron-deficient HF patients is highly cost-effective
Omecamtiv mecarbil might be less effective in patients with atrial fibrillation or flutter
Vericiguat effective irrespective of atrial fibrillation status
Baroreflex activation: a novel option to improve heart failure symptoms
Beta-blocker withdrawal to enhance exercise capacity in heart failure?
Inconclusive results for dapagliflozin treatment in heart failure
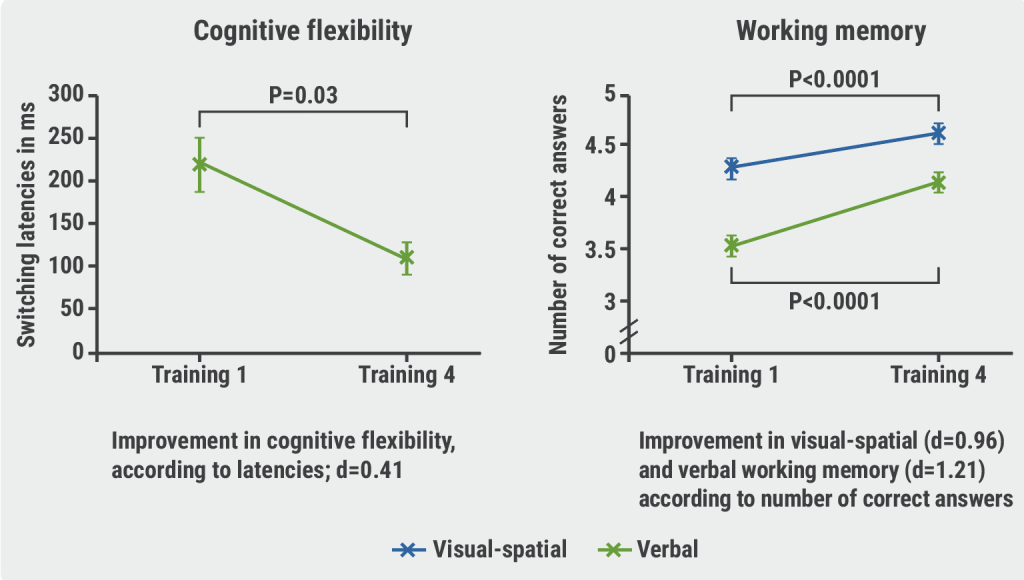
Computerised cognitive training improves cognitive function in HF patients
COVID-19 and the Heart
COVID-19-related HF: from systemic infection to cardiac inflammation
Myocardial infarction outcomes were significantly affected by the pandemic
TAPSE effective biomarker associated with high-risk of severe COVID-19
COVID-19 in AF patients with HF: no higher mortality but longer hospital stay
Cancer and the Heart
Heart failure patients might be at an increased risk for head and neck cancer
Trastuzumab associated with cardiotoxicity in breast cancer
Heart Failure Prevention and HRQoL in the 21st century
Psychoactive substances put young people at risk of cardiovascular disease
The challenge of improving the quality of life of heart failure patients
SGLT2 Inhibitors in Heart Failure
Empagliflozin linked to lower cardiovascular risk and renal events in real-world study
Efficacy of dapagliflozin and empagliflozin not influenced by diabetes status
Biomarker panel predicts SGLT2 inhibitor response
Best of the Posters
Real-world study suggests sacubitril/valsartan benefits elderly patients with HF
Proenkephalin: A useful biomarker for new-onset heart failure?
Weight loss associated with increased mortality risk in heart failure patients
Echocardiographic parameters linked to dementia diagnosis
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy