https://doi.org/10.55788/761fbd52
A placebo-controlled trial studying ravulizumab in NMOSD was deemed unethical because of the availability of eculizumab and other medications, explained Dr Sean Pittock (Mayo Clinic, MN, USA) [1]. A non-inferiority trial was unfeasible due to the rarity of AQP4+ NMOSD. Instead, the CHAMPION-NMOSD trial (NCT04201262) used the placebo group from the PREVENT trial (NCT01892345) investigating eculizumab. Propensity scores were used to account for potential confounders introduced by this comparator. Ravulizumab binds the same complement component 5-epitope as eculizumab, but has a longer elimination half-life, allowing for an extended dosing interval of 8 rather than 2 weeks.
Participants aged 18 years or older received a weight-based, IV loading dose of ravulizumab (2,400–3,000 mg) on day 1, followed by weight-based maintenance doses (3,000–3,600 mg) on day 15 and once every 8 weeks thereafter. The 58 participants on ravulizumab and 47 on placebo had a mean follow-up of 73.5 and 36.0 weeks, respectively.
The study met its primary endpoint, which was the time to first adjudicated, on-trial relapse and relapse-risk reduction (RRR). There were 0 on-trial relapses in the ravulizumab group versus 20 in the placebo group (P<0.0001), representing an RRR of 98.6%. The percentage of relapse-free participants at 48 weeks was 100% with ravulizumab and 63% with placebo. A key secondary efficacy endpoint, the adjudicated on-trial annualised relapse rate (ARR), was 0.00 with ravulizumab. This was superior to a predefined comparator ARR of 0.25 as well as the ARR of 0.42 in the placebo group (see Table for all secondary outcomes).
Table: Secondary endpoint results of the CHAMPION-NMOSD trial [1]

aBecause statistical significance for clinically important change from baseline in EQ-5D score was not met, P-values for the subsequent lower-ranking secondary endpoints are not significant; therefore, nominal P-values are presented.
ARR, annualised relapse rate; CI, confidence interval; EDSS, Expanded Disability Status Scale; HAI, Hauser Ambulation Index; N/A, not applicable; SD, standard deviation; VAS, visual analogue scale.
Ravulizumab was well tolerated, with a safety profile consistent with that of eculizumab. No unexpected patterns were observed in the treatment-emergent adverse events, which were reported in 93.1% versus 95.7% of participants in the experimental and placebo group, respectively. Serious adverse events were seen in 13.8% versus 55.3% of the participants. There were 2 cases of meningococcal infection in the ravulizumab group, which recovered with no sequelae. Their occurrence does highlight the need for close monitoring and risk evaluation.
- Pittock SJ. Efficacy and safety of ravulizumab in adults with anti-aquaporin-4 antibody positive neuromyelitis optica spectrum disorder: outcomes from the phase 3 CHAMPION-NMOSD trial. Abstract O051, ECRIMS 2022, 26–28 October, Amsterdam, the Netherlands.
Copyright ©2022 Medicom Medical Publishers
Posted on
Previous Article
« NMOSD patients are cognitively impaired regardless of serostatus Next Article
Humoral and cellular immune responses after SARS-CoV-2 vaccination »
« NMOSD patients are cognitively impaired regardless of serostatus Next Article
Humoral and cellular immune responses after SARS-CoV-2 vaccination »
Table of Contents: ECTRIMS 2022
Featured articles
Letter from the Editor
Diagnosis and Prediction of Disease Course
A case for including optic nerve lesions in the McDonald criteria
Cerebrospinal fluid kappa-free light chains for MS diagnosis
Early, non-disabling relapses increase disability accumulation
Physical impairment is present before perceived MS onset
Chronic active MS lesions respond poorly to anti-CD20 antibodies
Treatment: Trials & Strategies
Dimethyl fumarate reduces the risk of a first clinical event in RIS
How and when to make a timely switch to high-efficacy DMT
Comparing real-world effectiveness of DMTs
Study fails to show non-inferiority of rituximab to ocrelizumab
Autologous haematopoietic stem cell transplantation versus DMTs
Progressive MS
Stem cell transplantation not superior to natalizumab in progressive MS
Efficacy of DMTs fades away in secondary progressive MS
Smartphone tapping can help detect progressive MS
Paediatric MS
Early treatment with DMT effective in paediatric-onset MS
Fingolimod in paediatric MS: results of up to 6 years
Switching treatment after initial platform injectable DMT: real-world data
Pregnancy
Pregnancy and infant outcomes in women receiving ocrelizumab
New safety data of anti-CD20 mAbs around pregnancy
MS activity and pregnancy outcomes after long-term use of natalizumab
NMOSD
Ravulizumab significantly reduced relapses in AQP4+ NMOSD
NMOSD patients are cognitively impaired regardless of serostatus
Evidence-based consensus on pregnancy in NMOSD
COVID-19
COVID-19 and MS: lessons learned thus far
Ocrelizumab and fingolimod increase the risk of COVID-19 and of worse outcomes
Humoral and cellular immune responses after SARS-CoV-2 vaccination
Miscellaneous
Re-myelination strategies in MS still pose many unanswered questions
MS associated with a broader Epstein-Barr virus specific T-cell receptor repertoire
Cognitive rehab and mindfulness reduce cognitive complaints in MS
Related Articles
December 19, 2022
Physical impairment is present before perceived MS onset
November 25, 2020
Retinoid-X receptor agonist promotes remyelination
December 20, 2022
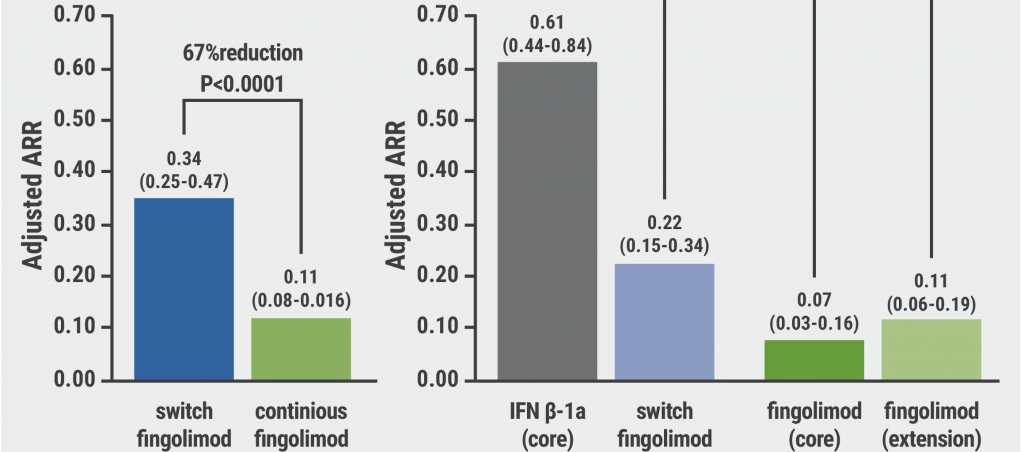
Fingolimod in paediatric MS: results of up to 6 years
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy
HEAD OFFICE
Laarderhoogtweg 25
1101 EB Amsterdam
The Netherlands
T: +31 85 4012 560
E: publishers@medicom-publishers.com

