https://doi.org/10.55788/ae6d06cb
PFA is a novel, non-thermal energy source for PVI. Although it is known that thermal energy sources affect the entire atrial tissue during PVI, including nerves and ganglia, the specific impact of PFA on neurocardiac tissue has not yet been investigated [1]. The current study randomised patients undergoing their first PVI (n=56) 1:1 to PFA or cryoballoon ablation. High-sensitive troponin I levels, indicative of myocardial damage, were assessed as well as S100b levels, a measure for neurocardiac damage. The postinterventional increase in heart rate, which is associated with neurocardiac damage, was also analysed. Dr Marc Lemoine (University Heart & Vascular Center Hamburg, Germany) presented the results [2].
S100b levels were 2.9 times lower in the PFA arm than in the cryoballoon ablation arm (P<0.001), suggesting that neurocardiac damage was reduced in the PFA arm. High-sensitive troponin I levels were 3.3 times higher in the PFA arm than in the cryoballoon ablation arm (P<0.01), which indicates that the damage to cardiomyocytes is increased with PFA compared with cryoballoon ablation for PVI. In addition, the ratio of S100b/troponin was reduced for PFA compared with cryoballoon ablation (P<0.01), suggesting that less neurocardiac damage was inflicted per lesion size (see Figure). Furthermore, a post-interventional increase in heart rate was not observed in patients who received PFA, whereas patients who were subjected to cryoballoon ablation showed a significant increase in post-interventional heart rate compared with patients who received PFA (P<0.01).
Figure: S100b/Troponin ratio for PFA and cryoballoon ablation [2]
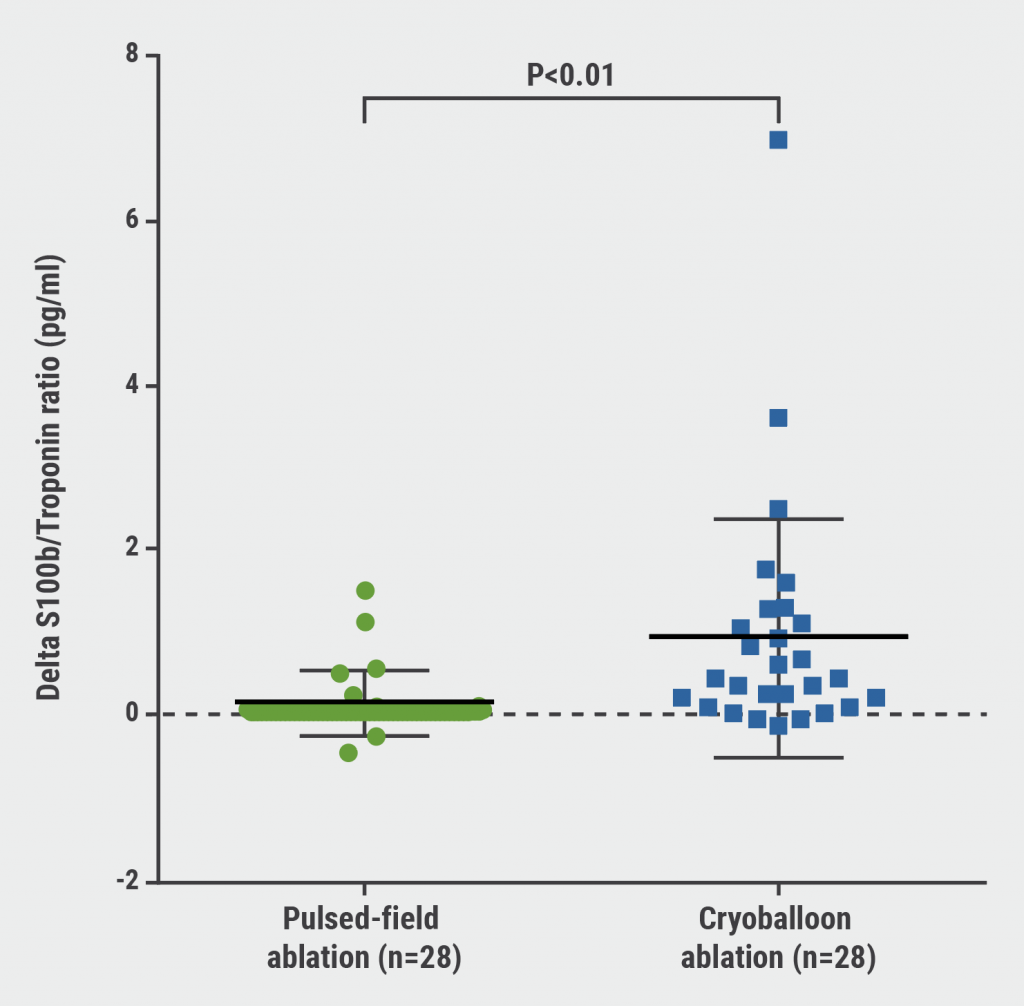
“This study validates the experimental concept that PVI by PFA leads to more specific damage to cardiomyocytes than to cardiac ganglia. We observed the loss of post-interventional increase in heart rate in patients who underwent PFA for PVI compared with those who underwent cryoballoon ablation for PVI,” concluded Dr Lemoine.
- Di Monaco A, et al. J Cardiovasc Dev Dis. 2022;9(4):94.
- Lemoine M, et al. Pulmonary vein isolation by pulsed-field ablation induces smaller neurocardiac damage than cryoballoon ablation. Atrial fibrillation and ablation, EHRA 2022, 3–5 April, Copenhagen, Denmark.
Copyright ©2022 Medicom Medical Publishers
Posted on
Previous Article
« Ultrasound-guided femoral venipuncture reduces complications in catheter ablation Next Article
Low AF recurrence rates after PVI using pulsed-field ablation »
« Ultrasound-guided femoral venipuncture reduces complications in catheter ablation Next Article
Low AF recurrence rates after PVI using pulsed-field ablation »
Table of Contents: EHRA 2022
Featured articles
Letter from the Editor
Diagnostics and Prevention
Cardiac magnetic resonance imaging improves prediction of post-MI sudden cardiac death
AI model accurately predicts sudden cardiac death in overall population
AI model accurately discriminates between arrhythmias
Impact of AF screening on stroke prevention influenced by systolic blood pressure
Developments in Devices
Conduction system pacing potential alternative for biventricular pacing in heart failure
Left bundle branch area pacing is a feasible technique for HF and bradyarrhythmia
Focus on the efficacy of cardiac resynchronisation therapy in HF plus concomitant AF
RESET: No survival benefit of CRT-defibrillator over CRT-pacemaker in heart failure
Insertable cardiac monitors effective for AF detection in cryptogenic stroke
Updates on Ablation
First results of the POWER FAST III trial
Real-world safety results on pulsed-field ablation with pentaspline catheter
VANISH: Ablation reduces shock burden compared with anti-arrhythmic drug in ventricular tachycardia
Low AF recurrence rates after PVI using pulsed-field ablation
Pulsed-field ablation reduces neurocardiac damage versus cryoballoon ablation
Ultrasound-guided femoral venipuncture reduces complications in catheter ablation
News on Atrial Fibrillation
Sex differences revealed in AF determinants and AF progression
Early rhythm-control therapy efficacious in men and women with AF
Progression in remote app-based monitoring of atrial fibrillation
Other Topics
Benefits of SGLT2 inhibitors may extend beyond HF-associated outcomes
Related Articles
June 1, 2022
First results of the POWER FAST III trial
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy

