"Our aim was to go beyond traditional preserved/impaired classification dichotomy, purposing a new categorization of cognitive deficits in MS," Dr. Ermelinda De Meo of San Raffaele Scientific Institute in Milan told Reuters Health by email.
In a cross-sectional study, her team applied latent profile analysis (LPA) to neuropsychological data and magnetic resonance imaging (MRI) metrics to MS-related brain damage.
"By using MRI, we were also able to identify neuroanatomical substrates for each phenotype, substantiating data-driven cognitive findings with a biological basis," she said.
"Translated into clinical practice," she continued, "this categorization could help plan rehabilitative strategies tailored for each phenotype (and) may integrate the Expanded Disability Status Scale in defining clinical disability and support clinicians in treatment choices - for example, a patient transition to a more severe phenotype may suggest a switch in pharmacological treatment."
As reported in JAMA Neurology, Dr. De Meo and colleagues analyzed 1,212 MS patients (mean age, 41; 65% women) and 196 healthy controls with similar demographics. Participants underwent neurological and cognitive evaluation. A subgroup also underwent brain MRI.
LPA was used on cognitive test z scores to identify cognitive phenotypes.
The five cognitive phenotypes identified were: preserved cognition (19.4%); mild-verbal memory/semantic fluency (29.9%); mild-multidomain (19.5%); severe-executive/attention (13.8%); and severe-multidomain (17.5%).
Compared with the other phenotypes, patients with preserved cognition and mild-verbal memory/semantic fluency were younger (mean age, 36.5 and 38.2, respectively) and had shorter disease duration (mean 8 years and 8.3 years).
Corresponding data for the other phenotypes were: Mild-multidomain: mean age, 42.6 and mean disease duration, 12.8 years; severe-executive/attention: mean age, 42.9; mean disease duration, 12.2 years; and severe-multidomain: mean age, 44 and mean disease duration, 13.3 years.
Severe cognitive phenotypes were most common in patients with secondary progressive disease.
MRI evaluation revealed that compared with those with preserved cognition, patients with mild-verbal memory/semantic fluency had decreased mean hippocampal volume (5.42 mL vs. 5.13 mL; those with the mild-multidomain phenotype had decreased mean cortical gray matter volume (687.69 mL vs, 662.59 mL); and those with the severe-multidomain phenotype had extensive brain damage, with decreased volume in all the brain structures explored, except for nucleus pallidus, amygdala and caudate nucleus.
Dr. De Meo and her colleagues are currently developing an "automated and unbiased classifier" that would enable neuropsychologists to enter a patient's score on each test, and the classifier would return the phenotype, she said. "We invite all MS centers to collaborate with us."
Dr. Ahmed Obeidat, Director, Neuroimmunology and MS Fellowship Program at the The Medical College of Wisconsin in Milwaukee told Reuters Health by email, "The current work challenged a reductionist way of categorizing cognition in MS - i.e., preserved versus impaired."
"The new categorization helps us think about cognitive domains differently based on patient age, disease duration, and disease subtype," he said. "The finding that the highest proportion of the most severe cognitive phenotype was found in patients with secondary progressive MS is important. This finding may be telling us that we are missing an opportunity to intervene early to treat people with MS with medications that can exert a difference in cognitive functions."
That said, he added, because it is a cross-sectional study, "one can make no conclusions about changes in cognition over time." Further, the findings are unlikely to be generalizable to an international patient population because cognitive difficulties might differ.
In addition, he said, "the study did not account for the possible effects of MS treatments on the measured outcomes," nor did it show how the different neurophysiological test findings might affect people's lives. "For example, information on employment or career change due to cognitive or physical difficulties would have been helpful."
Dr. Adam Kaplin, Chief Scientific Officer for MyMD Pharmaceuticals Inc. in Baltimore and an adjunct faculty member in the departments of Psychiatry and Neurology at the Johns Hopkins University School of Medicine, also commented by email. Like Dr. Obeidat, he noted that the study lacks "a demonstration that the categories of cognitive impairment have functional relevance to people with MS."
Further, "the role of depression was not adequately addressed," he said, noting that up to half of MS patients will experience clinical depression, which itself can cause cognitive impairment. "Moreover, the cognitive impairment due to depression has been shown to be associated with structural brain changes, making it even more important to control for this variable."
Dr. Kaplin also noted that the cognitive tests used in the study are not routinely used in practice, take 90 minutes to complete and must be administered by trained professionals. The connection between the findings and cognitive rehabilitation, he added, is "purely speculative," given the cross-sectional nature of the study.
SOURCE: https://bit.ly/35fu3fF JAMA Neurology, online January 4, 2021.
By Marilynn Larkin
Posted on
Previous Article
« ACT-FAST cuts time to endovascular thrombectomy without over-triage Next Article
Mindfulness-based cognitive therapy may reduce risk of recurrent depression »
« ACT-FAST cuts time to endovascular thrombectomy without over-triage Next Article
Mindfulness-based cognitive therapy may reduce risk of recurrent depression »
Related Articles
December 9, 2021
Personality trait alterations in MS patients
July 30, 2019
McDonald Criteria MS often misapplied and misunderstood
November 25, 2020
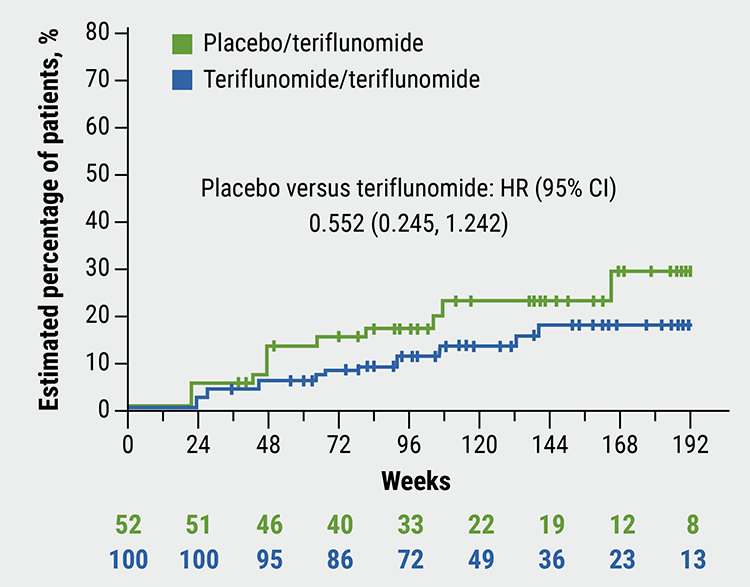
TERIKIDS trial extension of teriflunomide in paediatric MS
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy
HEAD OFFICE
Laarderhoogtweg 25
1101 EB Amsterdam
The Netherlands
T: +31 85 4012 560
E: publishers@medicom-publishers.com

