https://doi.org/10.55788/691730db
SELECT2 (NCT03876457) was a prospective, randomised, open-label, phase 3 clinical trial with blinded outcome assessment [1,2]. As 31 sites from the USA, Canada, Europe, Australia, and New Zealand participated, a covariate adaptive randomisation allowed for balanced baseline characteristics. Imaging evaluation was standardised. Participants were selected based on the presence of a stroke due to occlusion of the internal carotid artery or the first segment of the middle cerebral artery. The median ischaemic-core volume was ~80 ml (ranging from ~60 to ~120 ml). The 352 participants were randomised 1:1 to EVT plus medical care (n=178) or medical care alone (n=174). The median age was 67 years, and 73% were women. The primary outcome was the modified Rankin Scale (mRS) score at 90 days.
Leading author Dr Amrou Sarraj (UH Cleveland Medical Center, OH, USA) said that about 81% of patients in the control group had very poor outcomes at 90 days. The thrombectomy group saw a shift towards a more favourable outcome (see Figure). Dr Sarraj: “This shift translated into a 60% higher chance of improving the outcome on the mRS by at least 1 point.” (Wilcoxon–Mann–Whitney measure of superiority: 0.60). At 90 days, the generalised odds for achieving a better outcome on the mRS after thrombectomy versus medical care alone was significantly higher: odds ratio 1.51 (95% CI 1.20–1.89; P<0.001). A key secondary outcome was functional independence, which was not expected to be high in this population. It was met by 20% of participants in the thrombectomy group and 7% in the medical-care group (relative risk [RR] 2.97; 95% CI 1.60–5.51); the number needed-to-treat (NNT) was 7.34. The percentage of participants with independent ambulation in the thrombectomy group was 38% versus 19% (RR 2.06; 95% CI 1.43–2.96; NNT 5.11).
Figure: Modified Rankin Scale score at 90 days [1]
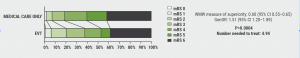
WMW, Wilcoxon–Mann–Whitney; CI, confidence interval; GenOR, generalised odds ratio.
Symptomatic intra-cerebral haemorrhage was infrequent and did not increase with thrombectomy (0.6%) versus medical management (1.1%; RR 0.49; 95% CI 0.04–5.36). Mortality was similar in the 2 groups: 38% versus 42% (RR 0.91; 95% CI 0.71–1.18). Early neurological worsening was increased, potentially related to infarct oedema. In the thrombectomy group, arterial access-site complications occurred in 5 participants, dissection in 10, cerebral-vessel perforation in 7, and transient vasospasm in 11 participants. Dr Sarraj concluded that these complications did not distract from the overall benefit of thrombectomy in this study population.
- Sarraj A. A randomized trial of endovascular thrombectomy versus medical management for ischemic stroke with a large core infarct on non-contrast CT or perfusion imaging. PL5.007, AAN 2023 Annual Meeting, 22–27 April, Boston, USA.
- Sarraj A, et al. N Engl J Med. 2023;388(14):1259–71.
Copyright ©2023 Medicom Medical Publishers
Posted on
Previous Article
« Continuous levodopa/carbidopa infusion shows favourable safety and efficacy Next Article
Harnessing the microbiome as a possible stroke treatment »
« Continuous levodopa/carbidopa infusion shows favourable safety and efficacy Next Article
Harnessing the microbiome as a possible stroke treatment »
Table of Contents: AAN 2023
Featured articles
Letter from the Editor
Positive results for hereditary transthyretin-mediated amyloid polyneuropathy
Infectious Diseases
Allogenic T-cell-based immunotherapy for PML in development
Cognitive Impairment and Dementia
Lecanemab may slow decline of cognition and function in Alzheimer’s Disease
Donanemab shows rapid and deep plaque clearance in early Alzheimer’s Disease
Epilepsy
Seizure forecasting and detection with wearable devices are feasible
Encouraging first results of GABAergic interneurons implants for focal epilepsy
Headache and Migraine
Lecture on migraine: from the prodromal phase to future paradigm shifts
Zavegepant nasal spray exhibits good efficacy and safety in acute migraine
A vaccine as a potentially safe and effective immunotherapy against CGRP
Multiple Sclerosis
Teriflunomide prevents conversion to MS in patients with RIS
Gold nanocrystals may be effective as adjunctive MS therapy
Muscle and Neuro-Muscular Disorders
First-ever ALS platform trial reports on outcomes of 4 treatments
Pridopidine for Huntington’s disease fails to meet the primary endpoint
Parkinson's Disease
Continuous levodopa/carbidopa infusion shows favourable safety and efficacy
Unilateral right STN-DBS improves verbal fluency
Stroke
Harnessing the microbiome as a possible stroke treatment
Patients with a large core infarct benefit from thrombectomy
Miscellaneous
Artificial intelligence applications in neurology: seize the moment
Spinal cord stimulation eases painful diabetic neuropathy
EVT improves functional outcomes in Chinese patients with BAO
Severe sleep apnoea associated with white matter hyperintensities
Related Articles
July 5, 2021
OSA: A risk factor for earlier cognitive decline
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy
HEAD OFFICE
Laarderhoogtweg 25
1101 EB Amsterdam
The Netherlands
T: +31 85 4012 560
E: publishers@medicom-publishers.com

