 Gout is a chronic disease of monosodium urate deposition characterised by arthritis flares and disability. Flares are inflammatory, often intensely painful, and debilitating, separated by asymptomatic intercritical periods. Advanced disease develops in approximately 15% of patients and is characterised by subcutaneous nodules composed of monosodium urate (tophi), unremitting articular inflammation, and potential joint erosion and deformity [2].
Gout is a chronic disease of monosodium urate deposition characterised by arthritis flares and disability. Flares are inflammatory, often intensely painful, and debilitating, separated by asymptomatic intercritical periods. Advanced disease develops in approximately 15% of patients and is characterised by subcutaneous nodules composed of monosodium urate (tophi), unremitting articular inflammation, and potential joint erosion and deformity [2].Chronic kidney disease (CKD) patients have a high prevalence and severity of gout. Pegloticase (pegylated recombinant uricase) rapidly metabolises urate and its efficacy is not impacted by CKD stage. Immunomodulator combination therapy with pegloticase has improved treatment response rates over phase 3 monotherapy trials by attenuating anti-drug antibodies. The MIRROR RCT trial (NCT03635957) met its primary endpoint treating uncontrolled gout in renal insufficiency patients with pegloticase and methotrexate [3]. The updated data presented at the ASN Kidney Week presented by Abdul Abdellatif, MD, FASN, board-certified nephrologist at Baylor College of Medicine and at CLS Health, TX, showed increased urate-lowering response rate (71.0% vs 38.5% during Month 6) and lower infusion reaction rate (4% vs 31%) in patients who received methotrexate over placebo in combination with pegloticase. In particular, the investigators measured the eGFR changes in MIRROR RCT from 100 patients randomised to pegloticase with methotrexate compared with 52 patients treated with pegloticase with placebo.
Doctor.webmd.com
In both treatment arms, eGFRs were stable during methotrexate or placebo run-in period and after pegloticase initiation (Day 1). At Week 24, eGFR had increased mildly in both groups, with a difference of +5.3±1.3 and +4.3±2.3ml/min/1.73m2 in the methotrexate (N=70; 69 responders) and placebo (N=19; 19 responders) groups, respectively, which was not significant. There were no differences in effect between subgroups of patients characterised by eGFR<60 versus ≥60 in either arm. The authors concluded that combination therapy with methotrexate was safe and effective for patients with and without pre-therapy eGFR <60ml/min/1.73m2; there was no evidence for negative impact on renal function in MIRROR RCT trial participants.
Medicom spoke with senior author of this presentation, Dr Bradley Marder, from Horizon Therapeutics, in Deerfield, Illinois.
Medicom: How should we interpret the new MIRROR RCT findings?
“I would say that the era of using pegloticase monotherapy for patients is over. We found that you can get both much better efficacy and much better safety using pegloticase with an immunomodulator medication like methotrexate. For those patients who have a kidney function that might not be able to tolerate methotrexate, physicians really need to look at other evidence, looking at other kinds of immunomodulator medications like mycophenolate mofetil, that has also been studied to prevent the development of anti-drug antibodies.
Likewise, I would also say that gout is not just a disease of intermittent inflammation in peripheral joints. Gout is a disease where monosodium urate does not just crystallise in the joints, but monosodium urate has been found to crystallise in just about every body tissue that there is. It is found in over 80% of coronary arteries and thoracic aortas of patients with gout, and that really does kind of illustrate the systemic and progressive nature of gout. Putting all the data together really gives us an urgency to identify patients who have gout and to make sure that they are treated effectively, whatever is needed.”
Medicom: What about patients who cannot tolerate methotrexate?
“The MIRROR RCT study was not in just patients with kidney transplants or patients with chronic kidney disease, but it is basically for all kidney disease patients with uncontrolled gout. The inclusion criteria for that trial were that a participant had serum uric acid above 7 mg/dL, patients who had failed to achieve treat to target goal of 6 mg/dL of uric acid on oral urate-lowering therapy, and they had to have some symptoms of gout, which could be 2 or more gout flares per year. In addition, we enrolled patients who were characterised by unresolving tophaceous disease, or with chronic gout with arthritis. All patients were randomised into the trial in a 2:1 format to either receive methotrexate, 15 milligrams orally once a week, or a placebo. We then studied the patients for a full year of pegloticase therapy, 8 mg by IV, every 2 weeks.
Notably in this trial, patients who had an eGFR <40 ml/min were excluded, not because you cannot use pegloticase in patients with chronic kidney disease, but because there was an abundance of caution to use methotrexate in patients with chronic kidney disease. Remember that methotrexate is a medication that is cleared by the kidney, and if you have chronic kidney disease, methotrexate concentrations can build up and cause a higher risk for either kidney injury, or other kinds of adverse events due to the accumulation of the medicine. Thus, patients with eGFRs <40 mL/min were excluded, but there were a sizable number of patients -roughly a third of all participants- who did have mild- to moderate-chronic kidney disease, or eGFRs between 40-60 mL/min.”
Medicom: What is the take-home message of the presentation at ASN?
“The overall results for the MIRROR RCT, the primary outcome data, were reported at the EULAR congress this last summer. Here at the ASN conference, we really wanted to focus on those patients who had chronic kidney disease enrolled in that trial.
In particular, we wanted to focus on what the impact of pegloticase and methotrexate would be on patients' kidney function and safety profile for those patients with chronic kidney disease. Some of the new data that was presented was not just the fact that the medication was effective for these patients, but also that the use of pegloticase and methotrexate did not negatively impact these patients' kidney function. So, we focused on eGFR levels before treatment, while they were in the run-in period with methotrexate, and for the 24 weeks duration of pegloticase therapy.
I always think of gout as being treated in 2 different ways. One approach is: what are you going to do with the inflammation, the pain that patients are experiencing? And often that inflammation is treated with anti-inflammatory medications, which are often either not effective in CKD patients, or are contraindicated, such as NSAIDs, for fear that they will negatively impact remaining kidney function. As a result, treating the inflammatory aspect of gout for most patients with moderate-to-severe chronic kidney disease is limited to steroids. We would all agree that steroids are just not a good medicine for patients over a prolonged period due to a high risk for side effects. In short, for tackling inflammation, we do not really have a lot of options for chronic kidney disease patients.
And similarly, for the chronic treatment of gout, which requires the lowering of serum uric acid levels, there are not such great options for CKD patients. Diet can help reduce serum uric acid levels a bit, maybe 1-2 mg/dL. But the thing about chronic kidney disease patients is the reason why they have high serum uric acid levels really does not have as much to do with the diet is the fact that their kidneys just do not have sufficient function to excrete the uric acid. Many medications to reduce serum urate levels are not effective, or can be even dangerous, to use in patients with chronic kidney disease for fear that uric acid concentrations within the renal tubule will increase and cause crystallisation of uric acid, causing kidney stone development.
Unfortunately, for patients with chronic kidney disease, febuxostat and allopurinol remain their only choices. However, with febuxostat getting a black box warning due to cardiovascular events, real-world evidence has shown us that allopurinol is primarily the only oral urate-lowering therapy that a lot of patients with chronic kidney disease receive. All in all, that means that particularly for patients with chronic kidney disease, who have such a high prevalence of gout, there are just not a lot of options available. I believe that this is why a lot of patients who end up with uncontrolled gout will require some kind of biologic therapy, like pegloticase.”
References
- Abdellatif, A. eGFR Changes in Uncontrolled Gout Patients Randomized to Receive Methotrexate or Placebo as Co-Therapy to Pegloticase: MIRROR RCT Findings. ASN Kidney Week, presented Nov 4, 2022. Abstract: SA-PO898.
- Mikuls TR. Gout. N Engl J Med. 2022 Nov 17;387(20):1877-1887.
- Botson JK, et al. A Randomized Placebo-Controlled Study of Methotrexate to Increase Response Rates in Patients with Uncontrolled GOut Receiving Pegloticase (MIRROR RCT): Primary Efficacy and Safety Findings. Arthritis Rheumatol. 2022 Sep 13. doi: 10.1002/art.42335. Epub ahead of print.
Copyright ©2022 Medicom Medical Publishers
Posted on
Previous Article
« Letter from the Editor Next Article
PROTECT trial: Pegloticase for Uncontrolled Gout in Kidney Transplant Recipients »
« Letter from the Editor Next Article
PROTECT trial: Pegloticase for Uncontrolled Gout in Kidney Transplant Recipients »
Related Articles
February 18, 2021
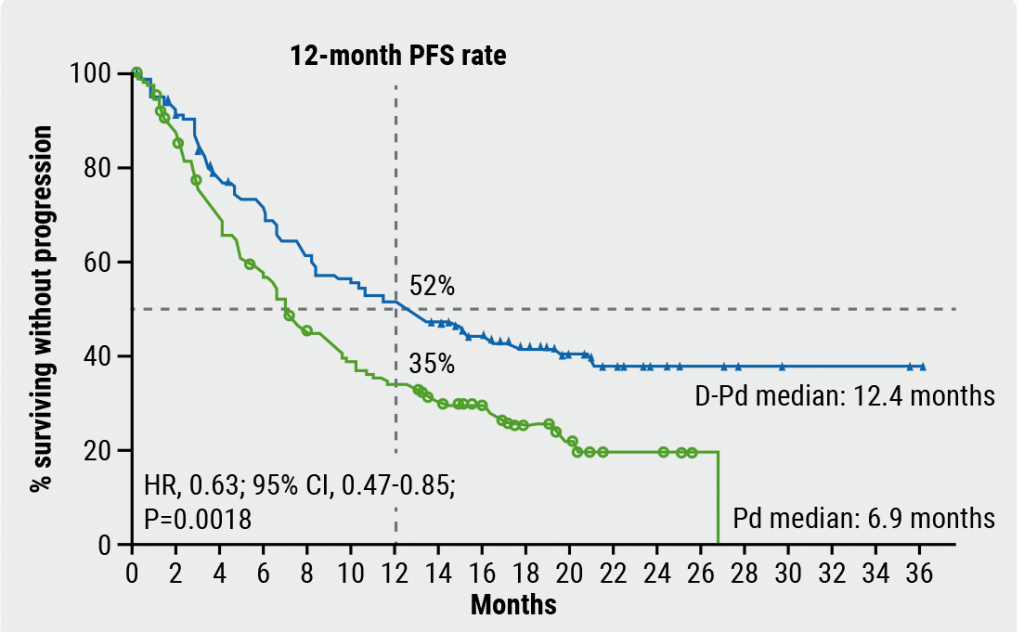
Subcutaneous daratumumab plus pomalidomide and dexamethasone in R/R MM
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy
HEAD OFFICE
Laarderhoogtweg 25
1101 EB Amsterdam
The Netherlands
T: +31 85 4012 560
E: publishers@medicom-publishers.com

