Radical surgery with or without cisplatin-based neoadjuvant chemotherapy is the current standard-of-care for muscle-invasive urothelial carcinoma. However, there is no conclusive level I evidence for adjuvant chemotherapy value with regard to OS, and only up to 50% of patients are eligible for cisplatin-based chemotherapy. Atezolizumab, an anti-PD-L1 antibody, is indicated as monotherapy in multiple locally advanced or metastatic urothelial carcinoma disease settings.
The IMvigor010 study evaluated the benefit of adjuvant atezolizumab versus observation in patients with high-risk muscle-invasive urothelial carcinoma of the bladder, renal pelvis, or the ureter [1]. Primary endpoint of IMvigor010 was DFS, secondary endpoint was OS. Patients were stratified by important clinical criteria, including number of lymph nodes resected, prior utilisation of neoadjuvant chemotherapy, lymph node status, tumour stage, and PD-L1 status. After stratification, patients were randomised 1:1 to atezolizumab (1,200 mg every 3 weeks for 16 cycles, or 1 year) or observation. There was no crossover allowed. The intention-to-treat population included 809 patients; in more than 90% the bladder was the primary tumour site. About half of the patients had received prior neoadjuvant chemotherapy. The very high-risk profile of the patient population was reflected by their pathologic stage, with patients having pathologic T-3 or T-4 disease in close to 40% of the patients in both arms, and 52% of the patients having node-positive disease.
Median DFS, the primary endpoint of IMvigor010, was 19.4 months in the atezolizumab arm versus 16.6 months in the observation arm. This difference did not translate into a significant hazard ratio (HR 0.89; 95% CI 0.74-1.08; P=0.244). There was no trend in favour of atezolizumab in any clinical or histochemical (PD-L1 expression) prespecified subgroup. OS results are not yet mature.
Overall, atezolizumab treatment was well tolerated. Treatment-related adverse events occurred in 71% of the atezolizumab arm. Treatment-related grade 3 or 4 events occurred in 16% of the patients in the atezolizumab arm. There was one episode of a grade 5 event that was attributed to atezolizumab that occurred in one patient. Adverse events leading to discontinuation of atezolizumab occurred in 16% of the patients.
- Hussain MHA, et al. ASCO Virtual Meeting, 29-31 May 2020, Abstract
Posted on
Previous Article
« First randomised trial of Lu-PSMA in mCRPC progressing after docetaxel Next Article
Novel drug for kidney cancers/VHL patients »
« First randomised trial of Lu-PSMA in mCRPC progressing after docetaxel Next Article
Novel drug for kidney cancers/VHL patients »
Table of Contents: ASCO 2020
Featured articles
COVID-19 & Telemedicine
COVID-19 and Cancer Consortium Registry: initial results
Oncology hospital-at-home model reduces hospitalizations, emergency department visits, and costs
Nurse-led telephone triage system reduces hospitalizations, helps patients manage symptoms at home
Melanoma
Adjuvant pembrolizumab: durable RFS for stage III melanoma
Pembrolizumab plus low-dose ipilimumab well tolerated after progression on PD1 antibody therapy
Toripalimab plus axitinib effective in metastatic mucosal melanoma
Breast & Ovarian Cancer
Advanced breast cancer: locoregional therapy does not improve OS
T-DM1 does not improve safety or efficacy in HER-2 positive early breast cancer; favorable iDFS reported
Maintenance olaparib improves OS in relapsed ovarian cancer with BRCA1/2 mutation
Combination pembrolizumab/chemo improves PFS in metastatic TNBC
Effect of veliparib with or without cisplatin in breast cancer: results of SWOG S1416
PHOEBE, a phase 3 trial comparing pyrotinib and lapatinib in HER2-positive metastatic breast cancer
BYLieve demonstrates efficacy of PIK3CA-directed treatment post CDK4/6-ihibition
Strategies emerge for chemotherapy de-escalation in HER2-positive breast cancer
Multiple Myeloma
Carfilzomib: no PFS benefit for multiple myeloma
Lung Cancer
ES-SCLC: tremelimumab + durvalumab + chemotherapy misses endpoint
Adjuvant osimertinib in NSCLC: practice changing ADAURA trial
ES-SCLC: pembrolizumab KEYNOTE-604 data
Second-line gemcitabine plus ramucirumab significantly improves overall survival
Tiragolumab and atezolizumab: ORR in NSCLC
MET-amplified advanced NSCLC responds well to MET inhibitor capmatinib
Genitourinary Cancer
Urothelial cancer: avelumab works as maintenance therapy
ARAMIS final OS and nmCRPC safety outcomes
Final survival results from phase 3 SPARTAN trial
Novel drug for kidney cancers/VHL patients
Primary analysis from IMvigor010, adjuvant atezolizumab in high risk muscle-invasive urothelial carcinoma
First randomised trial of Lu-PSMA in mCRPC progressing after docetaxel
Gastrointestinal Cancer
HER2-expressing metastatic colorectal cancer: trastuzumab deruxtecan
REGOMUNE: a phase 2 study combining regorafenib and avelumab
Cardiotoxicity: consider switching to S-1
Perioperative chemotherapy for resectable pancreatic ductal adenocarcinoma
Real-world data of sequential sorafenib followed by regorafenib in unresectable HCC
Paediatric Cancer
Sustained improvements in quality of life with larotrectinib
Promising first immunotherapy trial in placental trophoblastic tumours
Precision medicine for poor-prognosis paediatric patients
Related Articles
August 28, 2020
Carfilzomib: no PFS benefit for multiple myeloma
September 8, 2020
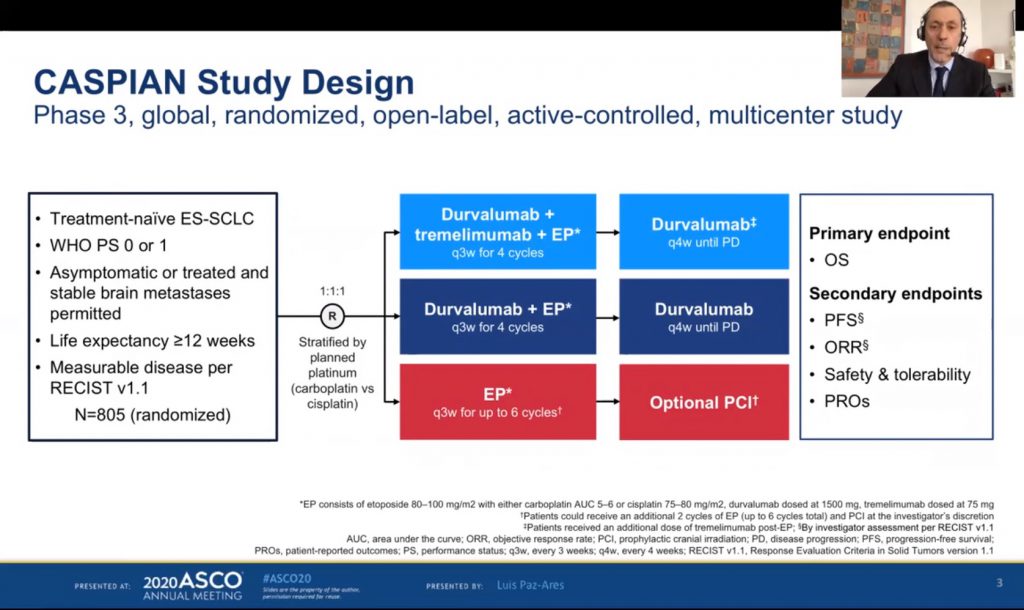
ES-SCLC: tremelimumab + durvalumab + chemotherapy misses endpoint
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy

