Neuromyelitis optica spectrum disorder (NMOSD), MOGAD, and MS have a different aetiology and pathogenesis and are difficult to differentiate clinically. The diagnostic gold standard for NMOSD and MOGAD is measuring aquaporin-4 and MOG antibodies, but sensitivity is limited and laboratory turnaround time is up to 2 weeks. There is a need for better and also quicker tests.
The objective of the presented study was to test whether NG-derived biomarkers in CSF could be used to differentiate NMOSD and MOGAD from MS and whether the results can be used for therapeutic decision-making in the acute disease phase. CSF samples were available of 42 patients with NMOSD (18 acute, 24 stable), 6 with MOGAD, and 41 with relapsing-remitting MS (18 acute, 23 stable). Four NG-markers were measured: elastase, MPO, MMP-8, and NGAL. They were compared with 2 known markers of neuronal (NfL) and astrocytic (GFAP) damage in NMOSD and MS, and with an additional astrocytic marker, i.e. S100B. CSF from 25 healthy controls served as reference.
The results showed that NG-markers appeared both in NMOSD and MOGAD. Their levels correlated both with the highest and lowest NG cell count in CSF. In acute NMOSD, all 4 NG-markers were increased compared to controls and acute relapsing-remitting MS (all P<0.01). Elastase, MPO, and MMP-8 were increased in MOGAD versus controls (P<0.025) and acute relapsing-remitting MS (P<0.04). GFAP levels were increased only in NMOSD, mainly in the acute phase (P<0.01). NfL was elevated in all disease groups compared with controls (P<0.01). Neither GFAP nor NfL were suitable as a diagnostic marker to distinguish between NMOSD and MS, but they can be useful disease activity markers. Increased S100B and GFAP levels differentiated acute NMOSD from MOGAD.
- Watanabe M, et al. Neutrophil granulocyte markers in cerebrospinal fluid differentiate NMOSD and anti-MOG antibody associated disease from MS in acute disease phase. MSVirtual 2020, Abstract LB01.03.
Posted on
Previous Article
« Eculizumab reduces long-term relapse risk in AQP4-positive NMOSD Next Article
Gut dysbiosis in NMOSD promotes CNS autoimmunity »
« Eculizumab reduces long-term relapse risk in AQP4-positive NMOSD Next Article
Gut dysbiosis in NMOSD promotes CNS autoimmunity »
Table of Contents: MS Virtual 2020
Featured articles
COVID-19 and MS
Biomarkers
Treatment Strategies and Results
Management of progressive MS with approved DMT
Novel Treatment Directions
Neuromyelitis Optica Spectrum Disorders
Miscellaneous Topics
Related Articles
December 20, 2022
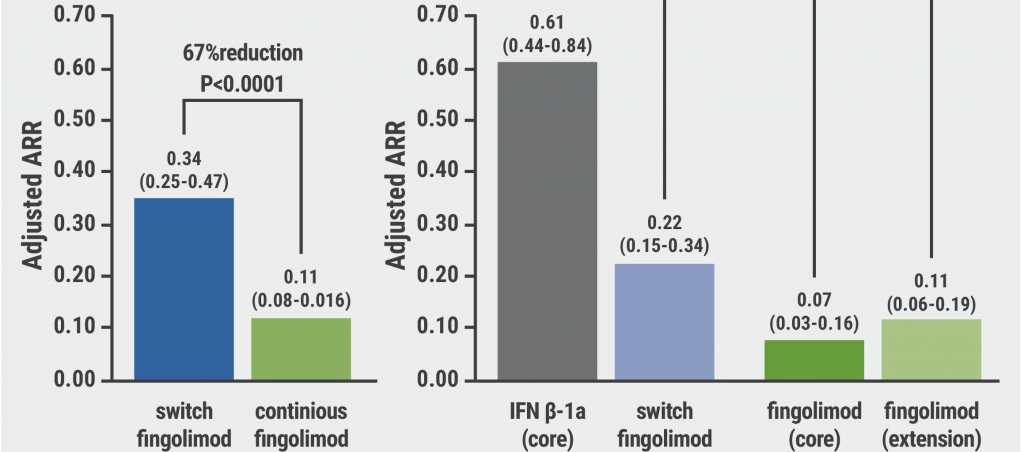
Fingolimod in paediatric MS: results of up to 6 years
December 16, 2020
Long-term safety and efficacy of ozanimod in relapsing MS
© 2024 Medicom Medical Publishers. All rights reserved. Terms and Conditions | Privacy Policy

